Discover the Power of Holistic Healing!
Being one of the leading Holistic Wellbeing and Wellness Studio in Newcastle, NSW, we take care of your overall health to help you lead a quality life. BPS Tensegrity Wellness Studio is a place where we are dedicated to nurturing your mind, body, and spirit.
Our studio offers a serene and inviting space, designed to create an oasis of calm amidst the hustle and bustle of everyday life. With a team of experienced practitioners, we provide a range of holistic services and practices, including yoga, meditation, massage therapy, nutrition counselling, and more.
Our approach is rooted in the belief that true wellness comes from addressing the interconnectedness of all aspects of your being. Join us on a transformative journey, where you can elevate your wellbeing, find balance, and unlock your fullest potential.
Our Rejuvenating Wellness Therapies
BPS Tensegrity Wellness Studio takes immense pride in offering transformative Wellness Therapies for Holistic Wellbeing in Newcastle!

Our Massage Therapy!
-
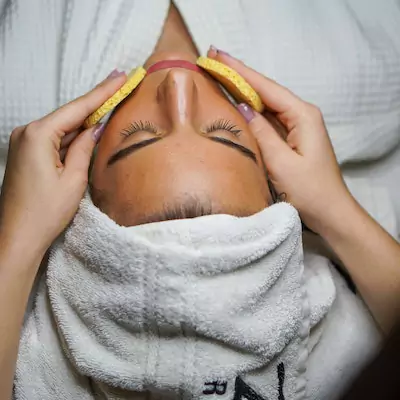
Experience the rejuvenating power of our massage therapy for holistic wellness. Our skilled therapists are dedicated to nurturing your mind, body, and spirit through the healing touch of massage.
-
With a variety of techniques, including Swedish, deep tissue, aromatherapy, and hot stone massage, we tailor each session to address your unique needs and promote deep relaxation.
-
Whether you seek relief from muscle tension, stress reduction, or a moment of pure bliss, our massage therapy will leave you feeling restored, revitalised, and balanced, supporting your overall wellbeing journey.

Unlock your body's natural healing potential with our transformative energy healing therapy. Our skilled practitioners utilise Reiki, chakra balancing, and intuitive techniques to restore energetic balance, promote deep relaxation, and support your overall wellbeing. Experience the profound benefits of energy healing as you rejuvenate your mind, body, and spirit on a profound level.

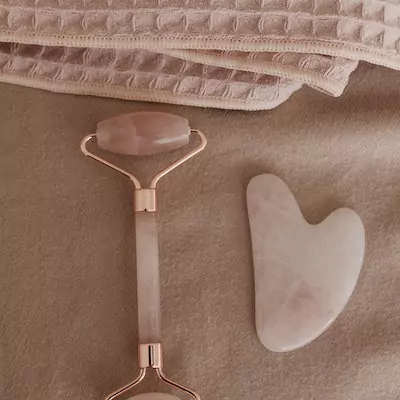
Indulge your senses and elevate your wellbeing with our aromatherapy sessions. Harnessing the power of natural essential oils, our skilled practitioners create a blissful environment that promotes relaxation, reduces stress, and enhances overall mood. Immerse yourself in the therapeutic aromas and experience the transformative effects of this rejuvenating therapy.
We are award-wining holistic wellbeing and wellness studio in Newcastle, NSW. We are dedicated to improving your mind and body health.

Discover the ancient healing art of acupuncture at our wellness studio. Our trained acupuncturists use gentle, precise needle placements to stimulate energy flow, promote balance, and address various health concerns. Experience the benefits of this holistic therapy and restore harmony within your body.
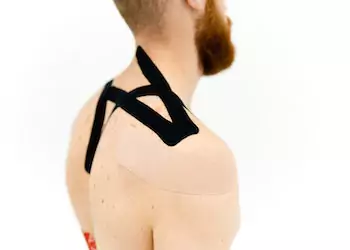
Experience the power of kinesiology at our wellness studio. Our skilled practitioners use muscle testing techniques to identify imbalances, release stress, and restore energy flow. Discover a personalized approach to healing and achieve greater physical, emotional, and mental wellbeing.

Embark on a journey of whole-body healing with our exceptional osteopathy services. Our highly skilled and compassionate osteopaths employ their expert touch and in-depth knowledge to restore balance, relieve discomfort, and enhance your body's innate healing capabilities.
Our Holistic Workout Sessions
Unleash Your Inner Power through our workout sessions and fuel your body!
Ignite your energy and boost cardiovascular fitness with our High-Energy Cardio sessions. These heart-pumping workouts incorporate dynamic exercises, interval training, and exhilarating music to get your heart racing and your endorphins flowing. Burn calories, build stamina, and discover your inner athlete in a fun and supportive environment.
Build functional strength and enhance overall athleticism with our Strength and Conditioning sessions. Led by experienced trainers, these sessions focus on resistance training, bodyweight exercises, and functional movements. Develop muscular strength, improve stability, and enhance your performance in daily activities and other physical pursuits.
Experience the joy of movement and express yourself through our Dance Fitness sessions. These energetic and uplifting workouts blend various dance styles, including Zumba, hip-hop, and contemporary, to create a fun and engaging fitness experience. Improve coordination, boost your mood, and unleash your inner dancer while getting a great workout.
At our holistic wellness studio in Newcastle, we offer invigorating Pilates sessions that focus on building core strength, improving flexibility, and cultivating a mind-body connection. Led by experienced instructors, our Pilates classes combine precise movements, controlled breathing, and body awareness to enhance posture, alignment, and overall body functionality.

Enjoy Vibrant & Holistic Life with Us!
Whether you're seeking relaxation, rejuvenation, or a path to personal growth, our studio is here to provide you with the nurturing and empowering experiences you deserve.
Taking Care of Your Health!
We prioritise your health by offering personalised services, expert guidance, and a nurturing environment, supporting your holistic wellbeing journey. To take this legacy forward we have listed our franchise on leading online platform to find health business for sale in Sydney, NSW , Newcastle and other regions of Australia. You can get all the information by visiting their website and apply for franchise opportunity. We support all our franchise with knowledge, manpower and setting up complete studio guidance by our experts.
-
Anxiety & Panic
Through tailored techniques and therapies, we aim to help you manage and reduce anxiety symptoms effectively.
-
Depression
We provide compassionate support and effective therapies for managing depression.
-
Headache
We offer targeted therapies for relieving headaches and promoting relaxation.
-
Gut Health
We offer holistic solutions to support and improve gut health.
-
Insomnia
We provide tailored approaches to promote restful sleep and combat insomnia.
-
Arthritis
We offer specialised therapies to alleviate arthritis pain and improve joint mobility.
-
Chronic Pain
We provide comprehensive approaches to manage and alleviate chronic pain effectively.
-
Mental stress
We offer holistic approaches to help manage and reduce mental stress.
-
Cervical
We provide specialised therapies to address cervical issues and promote neck health.
-
Pregnancy
We offer tailored wellness services to support a healthy and comfortable pregnancy journey.
Transformative Counselling Services
Our compassionate counsellors at BPS Tensegrity Wellness Studio offer tailored support to guide you through life's challenges, fostering resilience, and emotional well-being.
Individual Counselling
Our experienced counsellors provide one-on-one support, helping you navigate personal challenges, enhance self-awareness, and develop coping strategies for a more fulfilling life.
Couples Counselling
Strengthen your relationship and improve communication through our couples Counselling. Our skilled therapists facilitate healthy dialogue, promote understanding, and offer guidance for a harmonious and connected partnership.
Family Counselling
Our family Counselling services focus on fostering healthy dynamics, resolving conflicts, and improving communication within the family unit. Discover effective tools to strengthen relationships and promote a supportive family environment.
Stress and Anxiety Counselling
Our specialised counselors offer compassionate support to help you manage stress and anxiety. Through therapeutic techniques, learn coping strategies and develop resilience for a calmer and more balanced life.
We are honoured to have made a positive impact on our customer’s lives and remain dedicated to providing exceptional care and support for all who seek our services.

We are honoured to have made a positive impact on our customer’s lives and remain dedicated to providing exceptional care and support for all who seek our services.

We are honoured to have made a positive impact on our customer’s lives and remain dedicated to providing exceptional care and support for all who seek our services.

We are honoured to have made a positive impact on our customer’s lives and remain dedicated to providing exceptional care and support for all who seek our services.
Book your transformative session today and experience the profound benefits for yourself. Take the first step towards a healthier, happier you. Schedule your appointment now!

Discover the Power of Aromatherapy and Naturopathy!
Unlock the natural healing potential within you with the combined power of aromatherapy and naturopathy.
Tranquil Environment
Immerse yourself in a serene and calming atmosphere designed to enhance relaxation and promote a sense of peace during your therapy sessions.
State-of-the-Art Equipment
Our therapy section is equipped with the latest and most advanced tools and equipment to ensure optimal comfort and effectiveness in your wellness treatments.
Skilled Practitioners
Our studio is proud to have highly trained and experienced practitioners who provide expert guidance and personalised care to maximize the therapeutic benefits of your sessions.
Explore our insightful blog section, filled with valuable articles and tips on holistic wellness, self-care, and achieving a balanced lifestyle. Expand your knowledge and enhance your wellbeing.

Acupuncture is one of the most authentic and result-driven Chinese medicine or practice that consists of inserting fine needles into specific points on the skin. The purpose is to relieve pain and heal your body from mental and physical hardships. It has been gaining a lot of popularity among working…

Usually, a person’s lungs breathe in and out about 20,000 times each day. It is something people do without giving much thought. As simple as this might look, breathing is a procedure that requires the throat, nose, mouth, lungs, trachea, diaphragm, and other surrounding muscles to work collectively in tandem.…

After receiving the massage of your dreams, it is more than likely that you are immersed in a state of pure bliss. You may see the massage therapist in front of you, but you might be too relaxed to take in the words. It is more than likely that your…